
Breastfeeding After a Traumatic Birth - Tara's Story
Trigger Warning: This birth story discusses trauma, topics discussed include forceps delivery, postpartum haemorrhage, NICU and ICU, and post-natal anxiety and depression. If you are seeking support for your birth trauma, you may wish to contact Peer Support Service.
After a traumatic birth during the height of Melbourne’s COVID-19 lockdown, I struggled to breastfeed for reasons I was not expecting. Leading up to the birth, I armed myself with education, names of local lactation consultants, and joined breastfeeding support groups. I mentally prepared myself for tongue ties, latch issues and watched YouTube videos on hand expressing, ultimately only collecting 0.5 mls of colostrum in the unlikely event I would be separated from my baby. Unfortunately, that unlikely event became a reality.
My hopes for a home birth slipped away after two sleepless nights and nearly 12 hours of howling through contractions in the shower of my tiny apartment. With little to no progress in dilation and a transverse baby, I transferred to hospital. My daughter was born 12 hours later via forceps delivery. Despite exhaustion and shock, I brought my daughter immediately to my left breast. She was a dark shade of purple with swollen eyes and deep indents on her cheeks from the forceps blades. Hearing her cries, I couldn’t help but feel immediate guilt from the way in which she entered this world and that guilt engulfed me for many months following. Nevertheless, she immediately latched, and the world seemed to stand still, finally, for a few minutes.
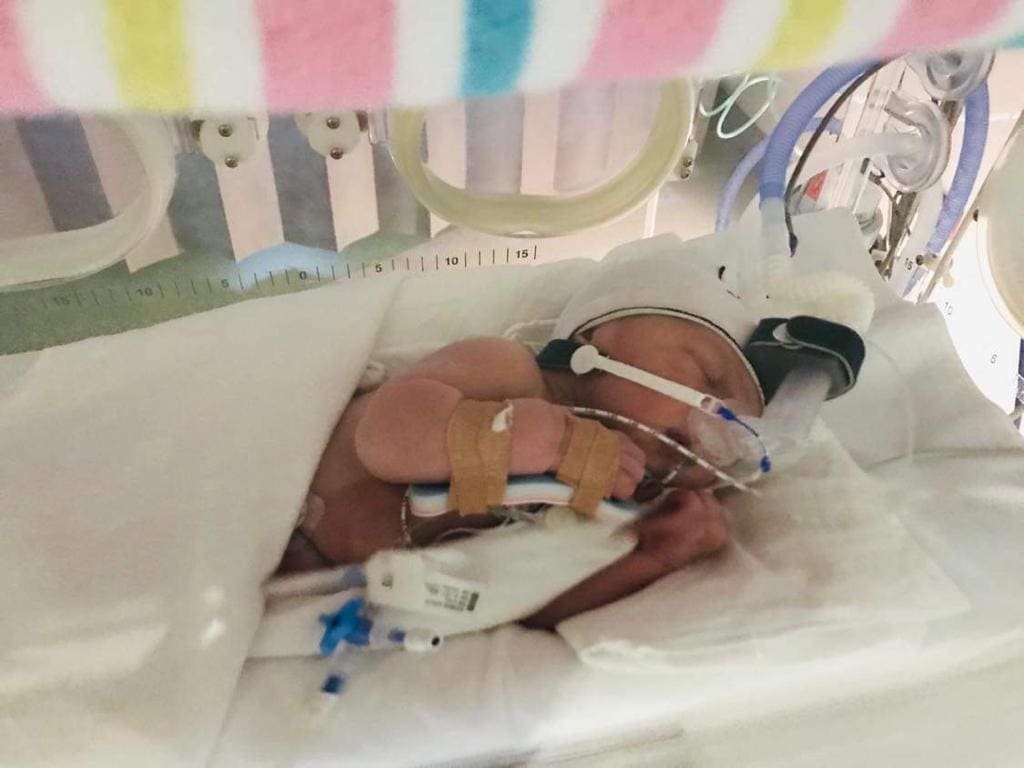
Unfortunately, my placenta wouldn’t detach, and I was rushed to theatre. The last thing I remember thinking as they wheeled me down the hallway was if my baby was okay, and what kind of support my partner would have if I didn’t survive. After a severe haemorrhage and infection from prolonged labour, I made it out of surgery. I was placed in critical care and my daughter in special care nursery a few floors above me. Unable to walk, I was wheeled up the next morning by nurses and saw my daughter in a humidicrib, wearing a cpap machine. She looked so helpless, and I knew she must have been so scared without me.
My pathetic 0.5 mls of colostrum wouldn’t have gone far and the nurses informed me they had been giving her sugar water to keep her calm. I immediately began breastfeeding her, trying to appreciate her, rather than focus on the cannula in her hand and the waves of shock that began to flood me. The lactation consultant told me that her latch looked deep, however within an hour or so there were concerns about my supply. Trying desperately to play catch up, I left my daughter on my breasts for as long and as often as I could. I woke up every three hours and wheeled myself up to special care nursery to feed her. Due to the significant blood loss, my milk took 8 days to finally come in and my colostrum wasn’t seeming to keep her calm. Discussions of formula began, and I dug my heels in. After several midwives tried to help me hand express, I finally asked if they had a pump, wondering why they hadn’t offered it earlier. I was able to pump and collect syringes of colostrum for her and she never ended up needing formula.
We were discharged after nearly a week, and my midwife came around to our home two days later. Concerned about weight loss, my midwife instructed me to pump and top up to speed things up. Between the cluster feedings, pumping, sleepless nights and coming to terms with the birth, I was in a terrible place. Having no family myself in Australia, my partner and I had no support. I got mastitis twice those first twelve weeks and began questioning flange sizes, tongue ties and my daughter’s latch. I saw a lactation consultant, which was just the beginning of a series of health issues for us. My daughter began to have gastrological symptoms of a suspected intolerance. We saw paediatricians and paediatric gastroenterologists, leading me to strict elimination diets and food journals. Despite already being vegan, I went on to remove soy, wheat, gluten, nuts, and coconut. Within a few months I lost several kilo’s and had only a handful of “safe” foods to eat. Hypoallergenic formula was discussed, and yet again I felt like a failure. After months of what I now recognise was severe Postnatal Depression, Anxiety and PTSD symptoms, I was at the end of my tether.
Whilst already at an all-time low, I received the diagnosis that I had pelvic organ prolapse. After months of asking midwives and physios why I feel so uncomfortable and heavy, I finally got the diagnosis I knew all along. I found myself doom scrolling the ambiguous world of prolapse at all hours of the night. Physios and doctors advised that upon succession of breastfeeding I’d see improvement in my prolapse and it’s symptoms, which felt like yet another inadvertent discouragement of our breastfeeding relationship.
Despite our hurdles, almost two years later we’re still going strong. Miraculously we were able to work through the separation, weight loss concerns, mastitis, food intolerances and everything in between. I’m sad that the months that were meant to be special were spent feeling unsupported, distracted and almost entirely unable to find joy in motherhood. However, after a long journey physically and psychologically, I’m in a much better place. I’ve been reluctant to publicly celebrate our accomplishment, as I’m aware it can be a painful reminder to others who were not able to breastfeed. Although I had seemingly a million valid reasons to stop, I’m glad I didn’t. Our breastfeeding journey was not easy, but in hindsight I think it enabled me to sit down and rest with my baby during times that I otherwise don’t think I would’ve allowed myself to. If I could tell newly postpartum Tara anything, it would be to believe people when they say it’s going to get better. It’s okay to not enjoy this period and it doesn’t make you a bad mother. Whatever your feeding journey, you and your baby will be okay and you’ll look back and be proud that you got through it.
If you would like to connect with someone after experiencing birth-related trauma, contact Peer2Peer Support service to connect with one of the Peer Mentors.
Read more

When you have a new baby, a lot of time and energy can be spent looking after your little one. However, it is crucial not to forget about yourself during this time. The postpartum period is delicat...

From self-care luxe items to the practical things that make life easier, buying a gift for a new mum – that she will actually use – helps her feel loved and supported, even from afar.













